aging
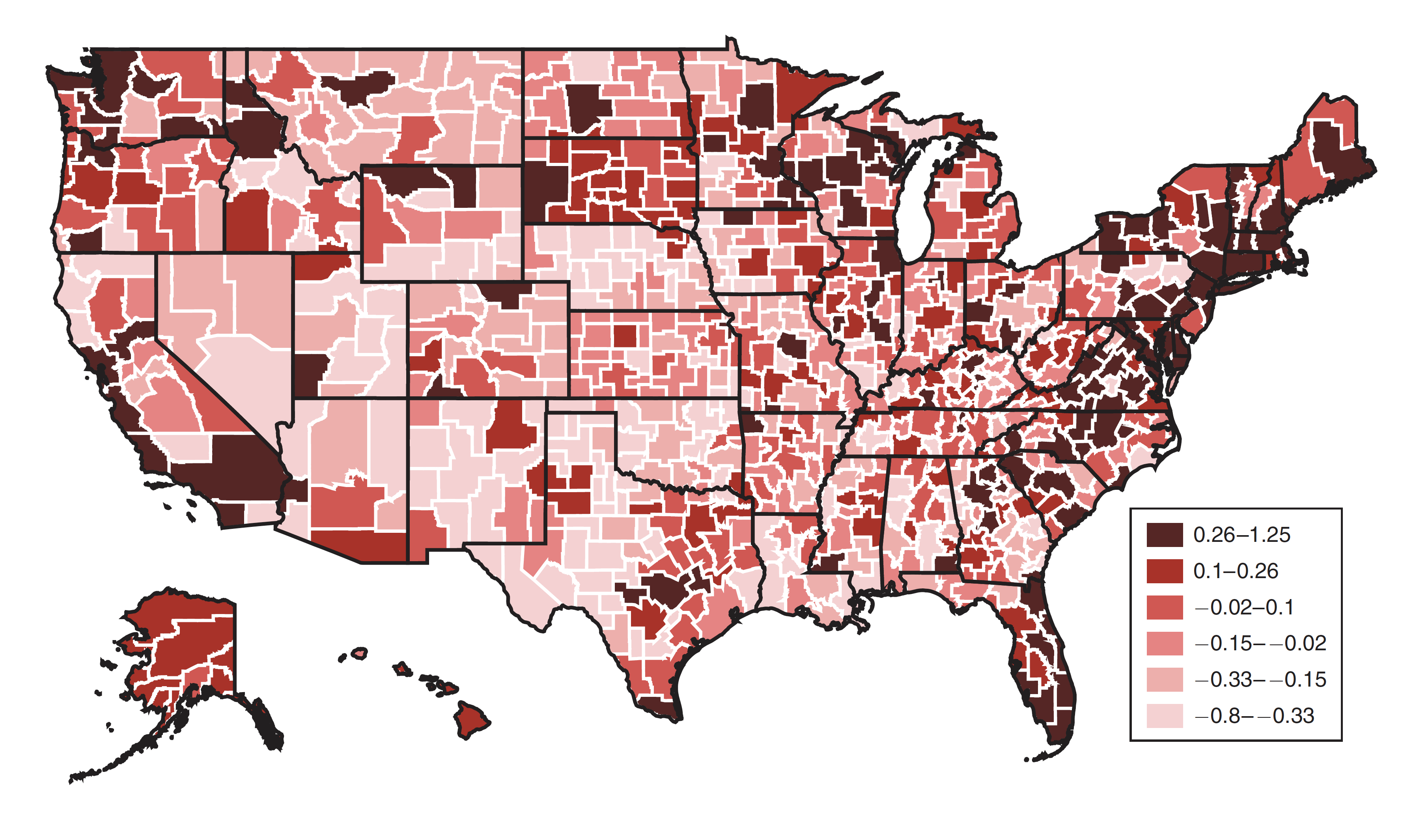
Longevity gets a new motto: location, location, location.
By slowing down aging, we could reap trillions of dollars in economic benefits.
Biomedical science assumes that people want to live as long as possible. They don’t.
Age ain’t nothing but a number, but “inflammatory age” may be real.
New machine-learning algorithms from Columbia University detect cognitive impairment in older drivers.
Older people are in grave danger of being left behind.
Researchers from Israel reversed two key processes involved in aging.
Research suggests that aging affects a brain circuit critical for learning and decision-making.
In fact, the maximum human lifespan has barely changed since we arrived.
The number of people with dementia is expected to triple by 2060.
Why a survey claims Boomers demonstrate more knowledge and safer behavior.
Researchers at University College London link waist circumference with dementia.
Did you know that shifting to a positive perspective on aging can add 7.5 years to your life? Or that there is a provable U-curve of happiness that shows people get happier after age 50?
▸
01:02:06 min
—
with
Volunteering can feel great and make good things happen. Now we know it promotes your health too.
A joint study by two England universities explores the link between sex and cognitive function with some surprising differences in male and female outcomes in old age.
It may be easiest when you’re young, but the proven benefits of learning a new language at any age cannot be ignored.
A Penn State study finds today’s middle-aged are experiencing much higher stress levels than 30 years ago.
Is the cult of youth what we really want trailing us into the afterlife?
How can we promote the creation of new neurons – and why is it so important?
A new study shows the benefits of calorie restriction. Never has such advice been more needed.
The Alzheimer’s Association says its new analysis and surveys “should sound an alarm regarding the future of dementia care in America.”
Increasing numbers of seniors need help with basic tasks. It doesn’t have to be that way.
“I used to mountain climb… If I can’t walk anymore, I’ll crawl.”
60 is the new 30, says Melanie Katzman. Embrace your age and the benefits that come with it.
▸
2 min
—
with
Researcher discovers a universal slump in life satisfaction.
A new study shows that altering the ISS and TOR pathways in roundworms can extend lifespan by 500 percent.
Embracing signs of age might be the road to a longer life after all.
Getting older — see: looking older — is not ideal in the workplace culture of youthfulness.
▸
3 min
—
with