dementia
Alzheimer’s has proved difficult to treat. But solving the mystery of this ultra-rare frontotemporal dementia may unlock new understanding.
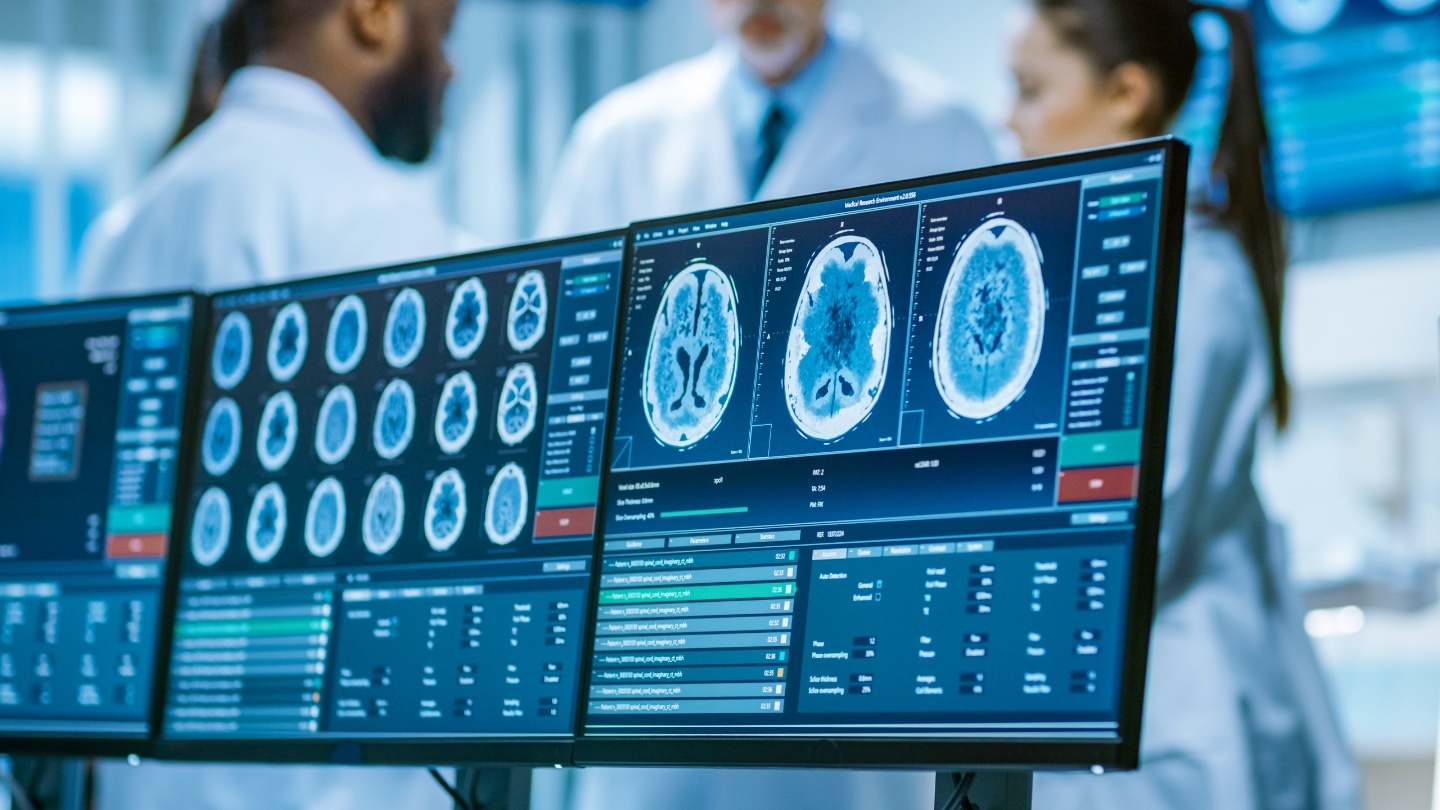
Researchers develop the first objective tool for assessing the onset of cognitive decline through the measurement of white spots in the brain.
Yet 80 percent of respondents want to reduce their risk of dementia.
Preliminary studies on mice show positive results.
Researchers at University College London link waist circumference with dementia.
The Alzheimer’s Association says its new analysis and surveys “should sound an alarm regarding the future of dementia care in America.”
The assumption “that without memory, there can be no self” is wrong, say researchers.
This means the disease may be curable and a vaccine possible.
One patient retained the ability to dress herself, make a simple meal, and even change her plans depending on the weather.
An international team of researchers claims to have found a major cause of dementia – an incurable brain disease.
The prevalence of Alzheimer’s disease is expected to triple over the next three decades, to nearly 14 million in the United States alone.
Research points to many social-cognitive, emotional, behavioral and biological benefits that marriage seems to bestow on its participants.
Scientists have developed an algorithm that reliably detects the signs of Alzheimer’s dementia before its onset.
A new study shows that being (and remaining) overweight and having type 2 diabetes is neurological nightmare.
Scientists identify key compounds that may help prevent brain diseases like Alzheimer’s, Parkinson’s, Huntington’s as well as Lou Gehrig’s disease.
New research by Australian scientists shows what exercise can make some people more intelligent and prevent dementia.
Robin Williams was trapped inside his own rapidly-deteriorating brain, which was being overtaken by what his wife refers to as a “terrorist” — Lewy Body Disease.