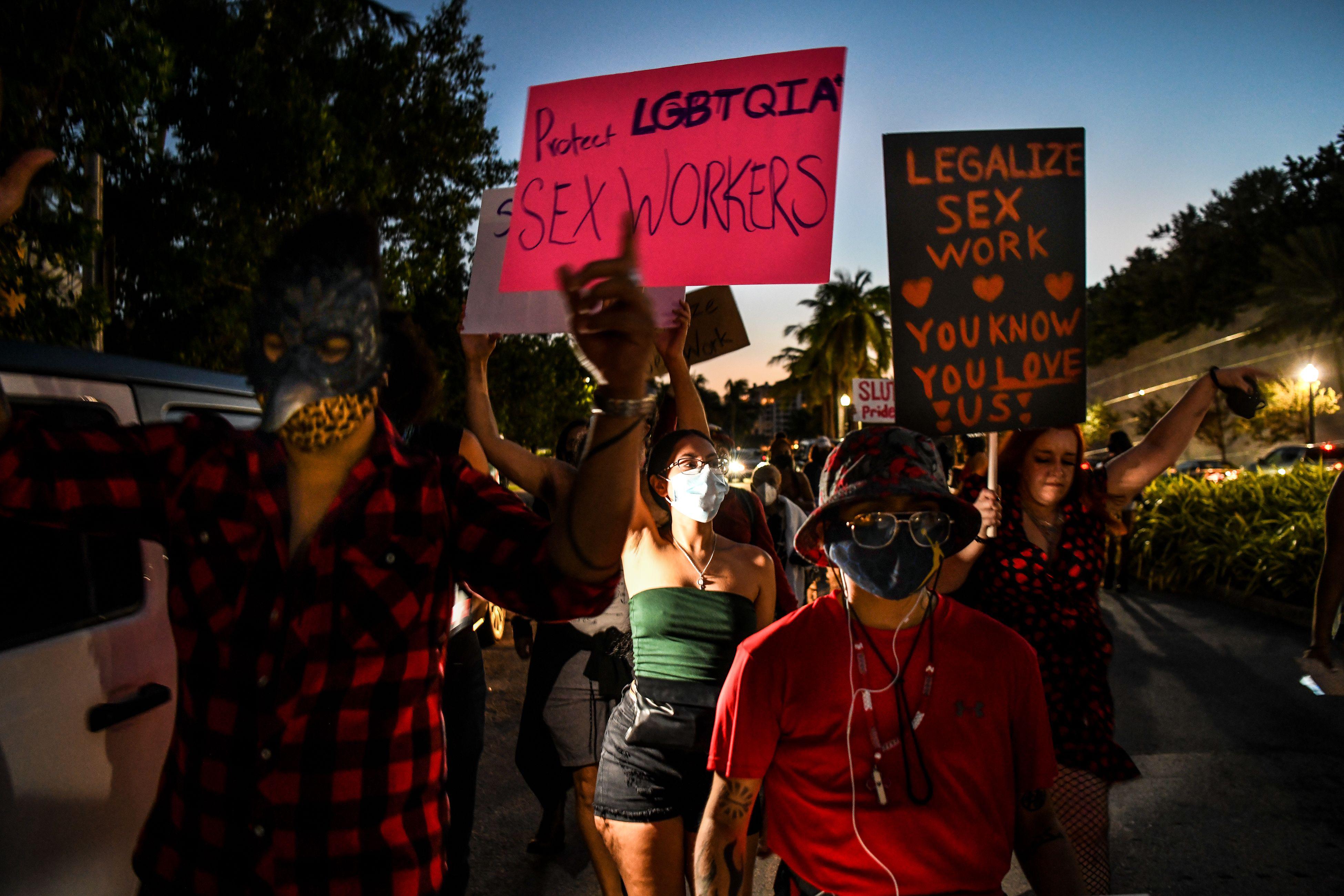public health
Timothy Caulfield, a leading science communicator, discusses the challenges of combatting misinformation in an age of information overload.
A food safety researcher explains another way to know what’s too old to eat.
Explore the key highlights from the UN’s latest release of its world population estimates.
Two ICU physicians offer a new approach to stopping it.
To reap the benefits of digital technologies, we must contend with their addictive designs.
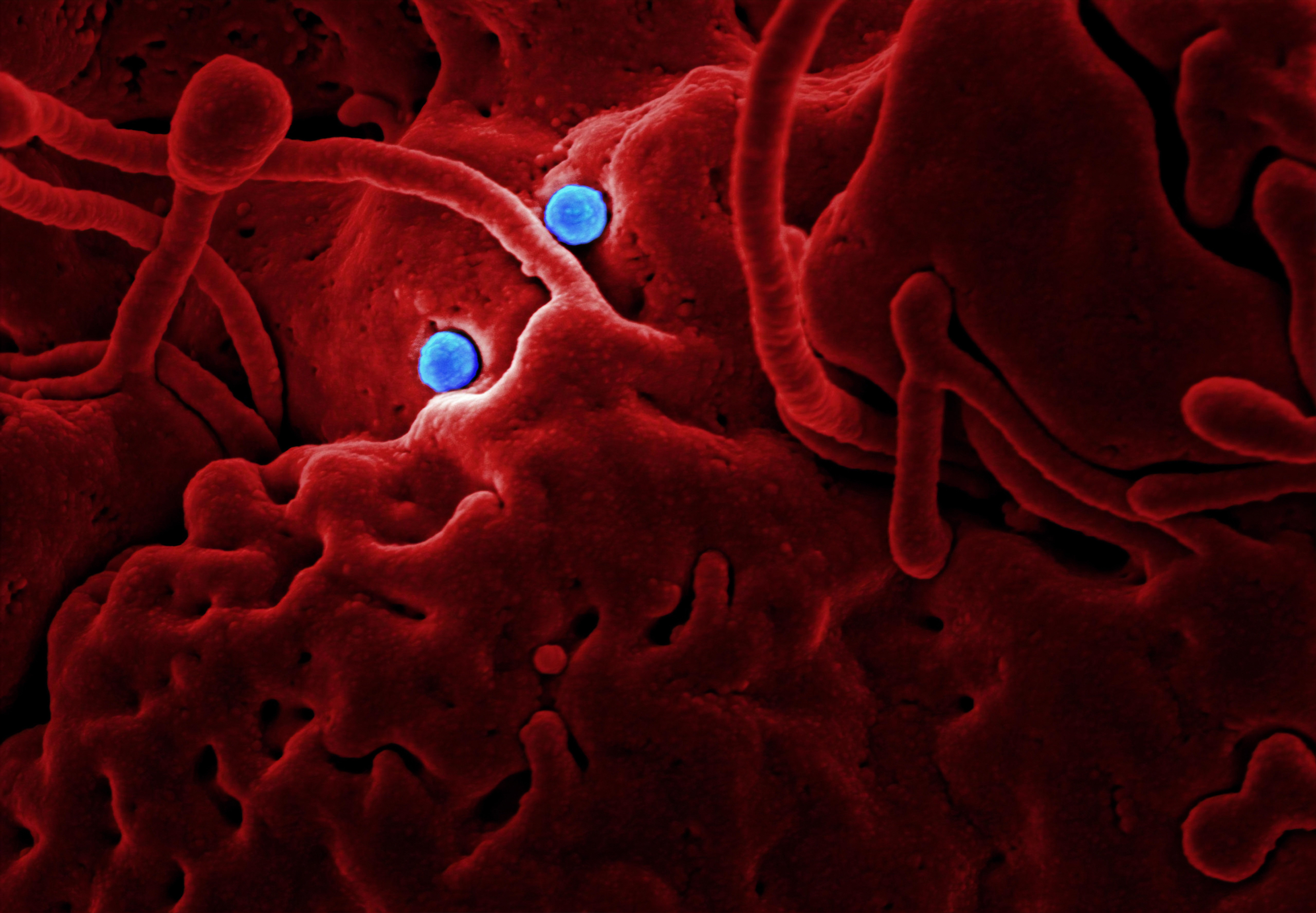
A new study looks at what happens when you get infected with two viruses at the same time.
Hospitals often deal with the aftermath of gun violence, but they can play a key role in preventing it.
▸
5 min
—
with
In ancient Greece, the Olympics were never solely about the athletes themselves.
Smallpox was nothing new in 1721.
Are you getting a full 8 hours?
A team of biohackers is on a David-versus-Goliath mission to make insulin affordable to an increasing number of diabetics.
New research shines a light on the genetics of sudden cardiac deaths.
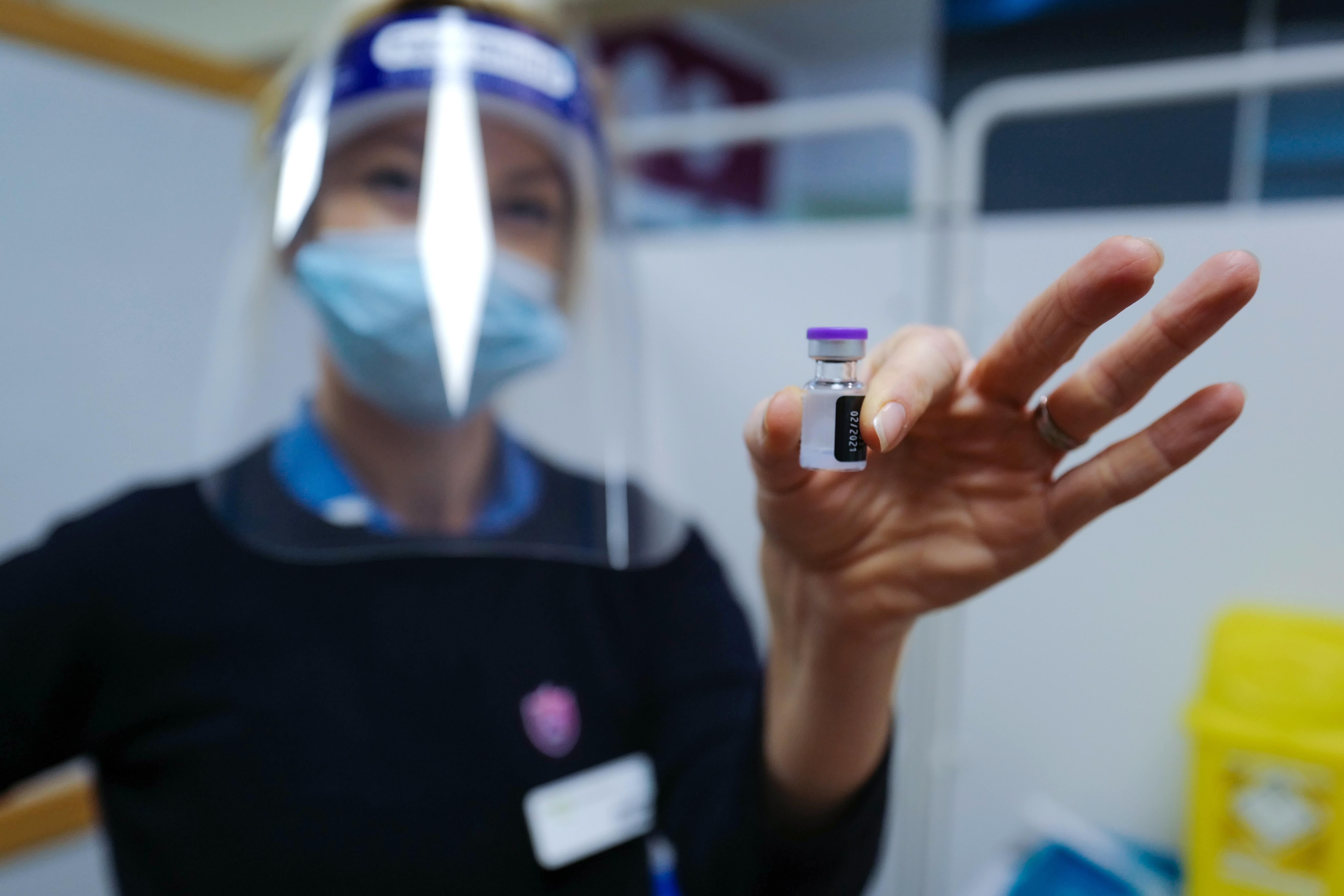
It could lead to a massive uptake in those previously hesitant.
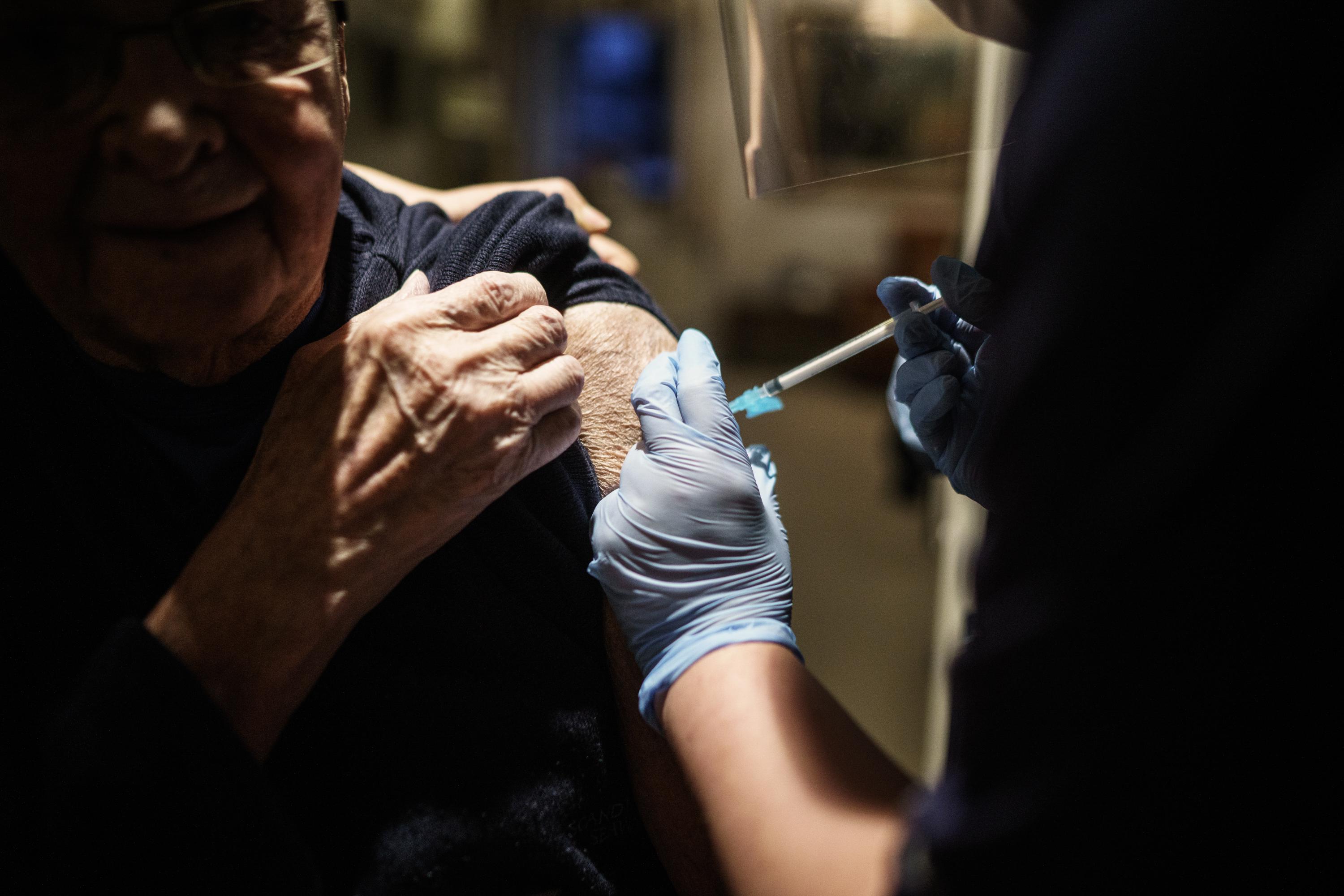
According to this research, eight percent of Americans always refuse vaccines. Why?
Virtual tourism has thus far been a futuristic dream, but a world shaped by Covid-19 may be ready to accept it.
Contact-tracing apps can be a useful tool for public health, but they have considerable false positive and false negative rates.
Noise causes stress. For our ancestors, it meant danger: thunder, animal roars, war cries, triggering a ‘fight or run’ reaction.
The pandemic has many people questioning whether they ever want to go back to the office.
The retraction crisis has morphed into a citation crisis.
The neoliberal call for more ‘choice’, seems hard to resist.
People may be more willing to get vaccinated when told how popular it is.
A psychologist and a doctor of emergency medicine explain.
Whose responsibility is it to ensure that there is affordable access to employment?
If we lose our pollinators, we’ll soon lose everything else.
The vaccine will shorten the “shedding” time.
One bill hopes to repeal the crime of selling sex and expand social services; the other would legalize the entire sex trade.
Remedies must honor the complex social dynamics of adolescence.
The majority of Americans are stressed, sleep-deprived and overweight and suffer from largely preventable lifestyle diseases such as heart disease, cancer, stroke and diabetes. Being overweight or obese contributes to […]
It’s not the caffeine; it’s the people.