poverty
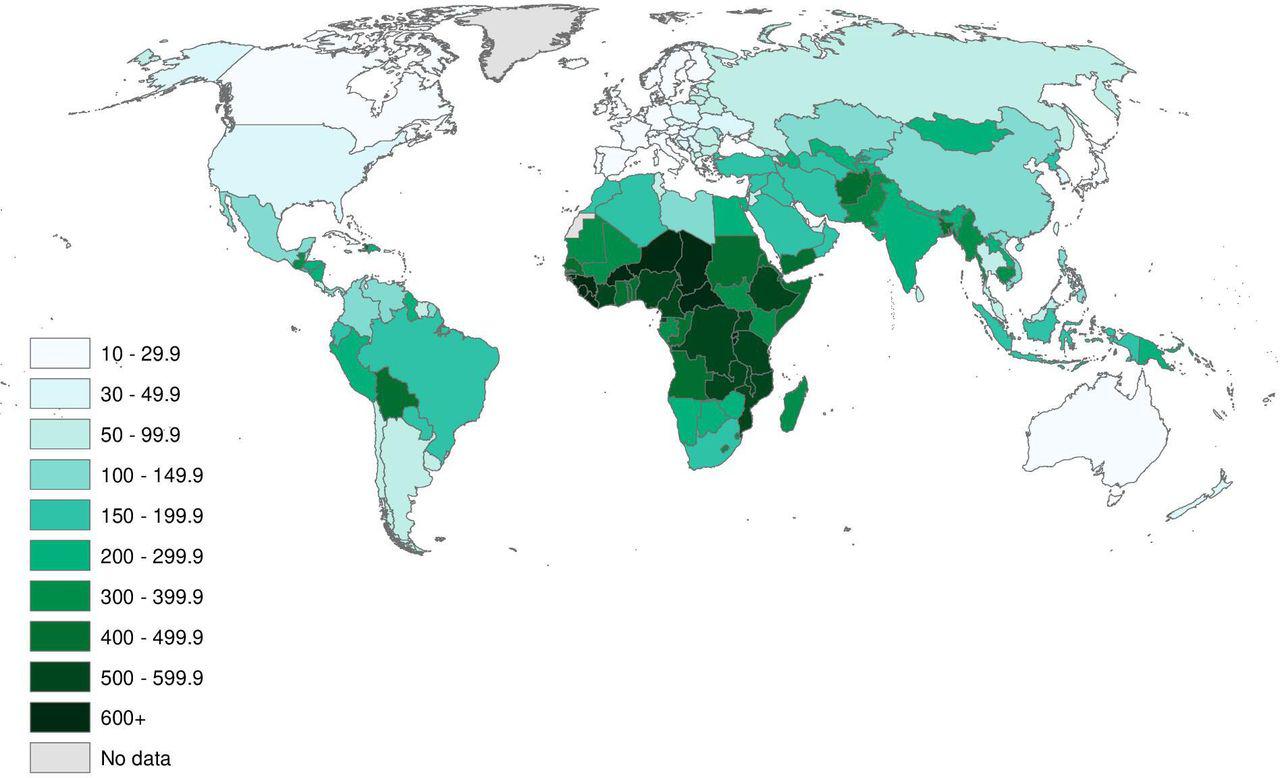
Nearly 90% of the world’s blind live in low-income countries.
It could lead to a massive uptake in those previously hesitant.
Healthy people need healthy microbiomes from an early age.
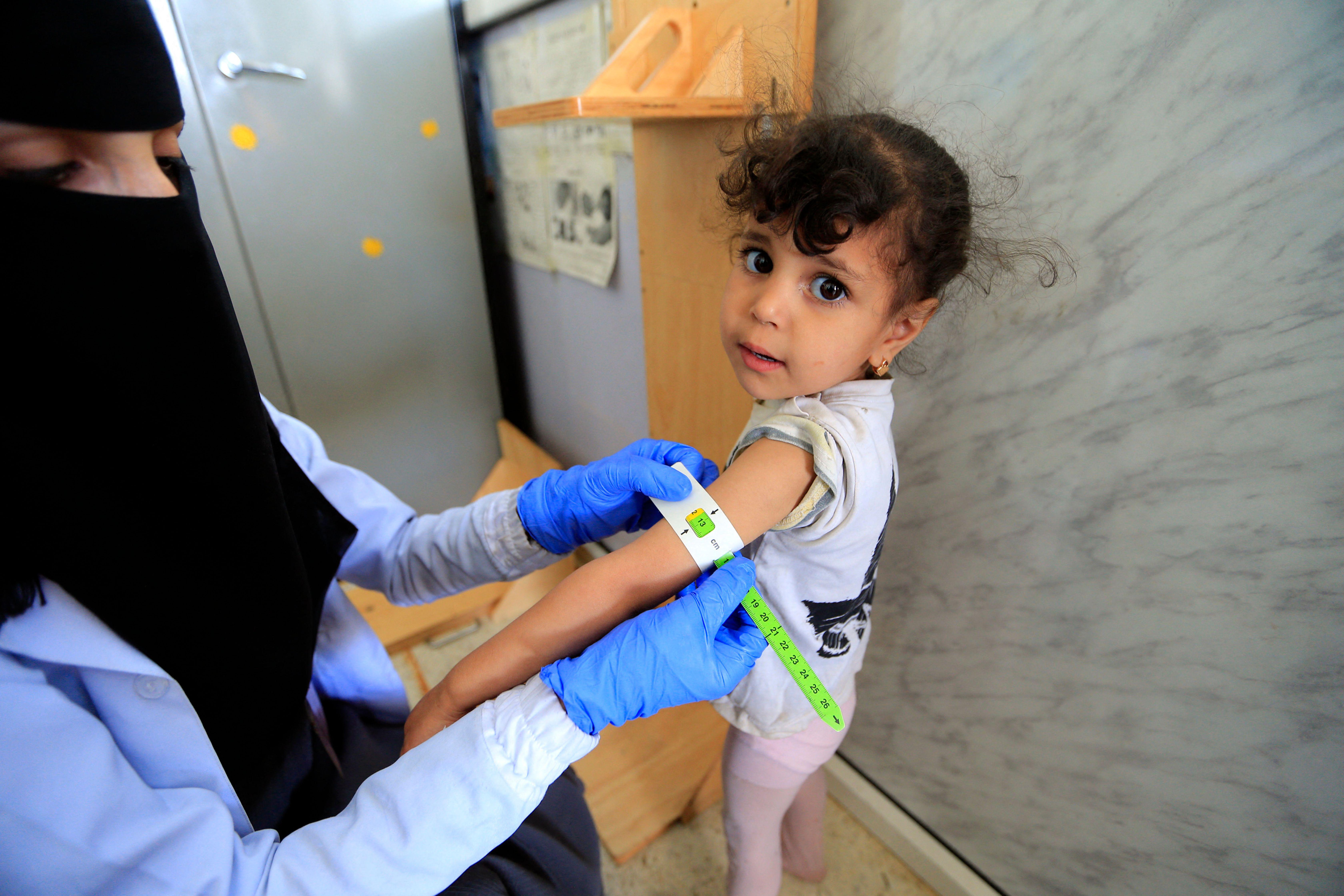
Global inequality takes many forms, including who has lost the most children
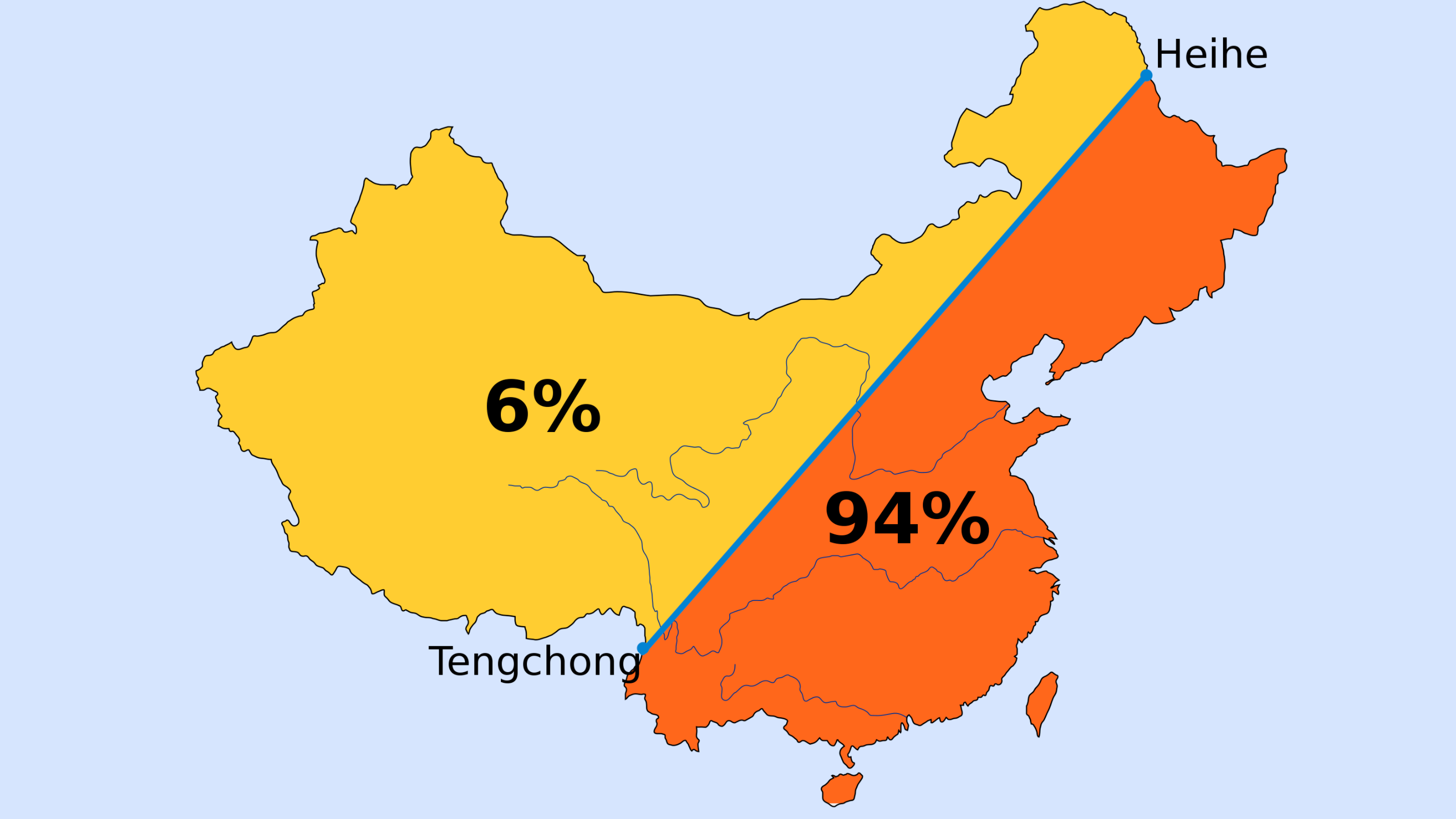
First drawn in 1935, Hu Line illustrates persistent demographic split – how Beijing deals with it will determine the country’s future.
Pandemics have historically given way to social revolution. What will the post-COVID revolution be?
Want to tell someone’s future in the US? You don’t need a crystal ball, just their zip code.
New research spotlights how low-income Black households face greater financial distress and vulnerability as a result of the pandemic economic crisis.
The next era in American history can look entirely different. It’s up to us to choose.
▸
5 min
—
with
The COVID-19 pandemic is making health disparities in the United States crystal clear. It is a clarion call for health care systems to double their efforts in vulnerable communities.
Monopolies wield an immense amount of economic and political power and influence. So what can we do to make the economy more equitable?
▸
5 min
—
with
A new study shows how poor children are negatively impacted neurologically.
Money can’t buy happiness, but try being hopeful and broke at the same time.
From reassessing the way schools are funded to changing the curriculum, there are ways to fix the inequities in education.
▸
4 min
—
with
The American economy may be locked into an unhealthy cycle that only benefits a select few. Is it too late to fix it?
▸
19 min
—
with
COVID-19 may strengthen the case for universal basic income, or an idea like it.
▸
24 min
—
with
OpenStax reimagined textbooks and saved students $1 billion. Now is a moment to reimagine even more. How can education help students learn more, better, and faster?
Should pharmaceutical companies pay people for their plasma? Here’s why paid plasma is a hot ethical issue.
▸
17 min
—
with
How will the current challenges to the global economy pressure it to change?
▸
4 min
—
with
The welfare state is broken. UBI is the smarter, more effective option.
▸
4 min
—
with
As it turns out, people who can afford to fly all the time use more energy than anybody else.
Deciding how we ought to live is one of the greatest challenges of being alive. Ask yourself these important questions to gain clarity, with philosopher Peter Singer.
▸
7 min
—
with
There are many different ways of helping people in extreme poverty. Philosopher Peter Singer explains how you can do it.
▸
5 min
—
with
Americans just want to pay their bills. Is universal basic income the path to financial stability and economic opportunity?
▸
5 min
—
with
Answer: When 22 men make more money than all of the women in Africa, an Oxfam study says absolutely.
Our personal choices can help to effectively combat poverty, says Peter Singer.
▸
7 min
—
with
Millennial income did not recover from the Great Recession like older generations’, a disparity that can have dire consequences for future generations.
There is greater social distance between Americans than ever before.
▸
2 min
—
with
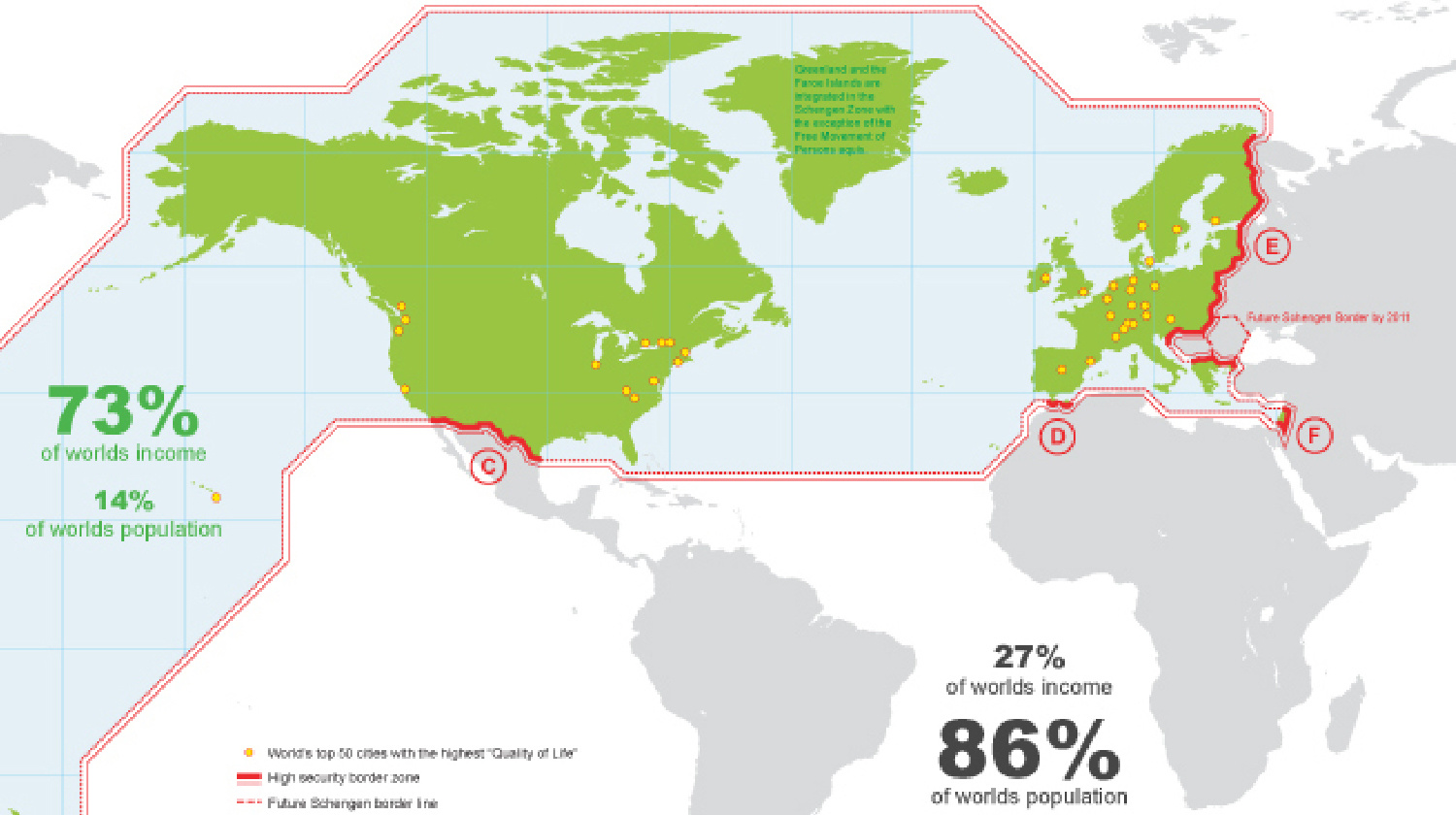
A review of the global “wall” that divides rich from poor.