epidemiology
A Harvard professor’s study discovers the worst year to be alive.
A newly discovered coronavirus — but not the one that causes COVID-19 — has made some dogs very sick.
A psychologist and a doctor of emergency medicine explain.
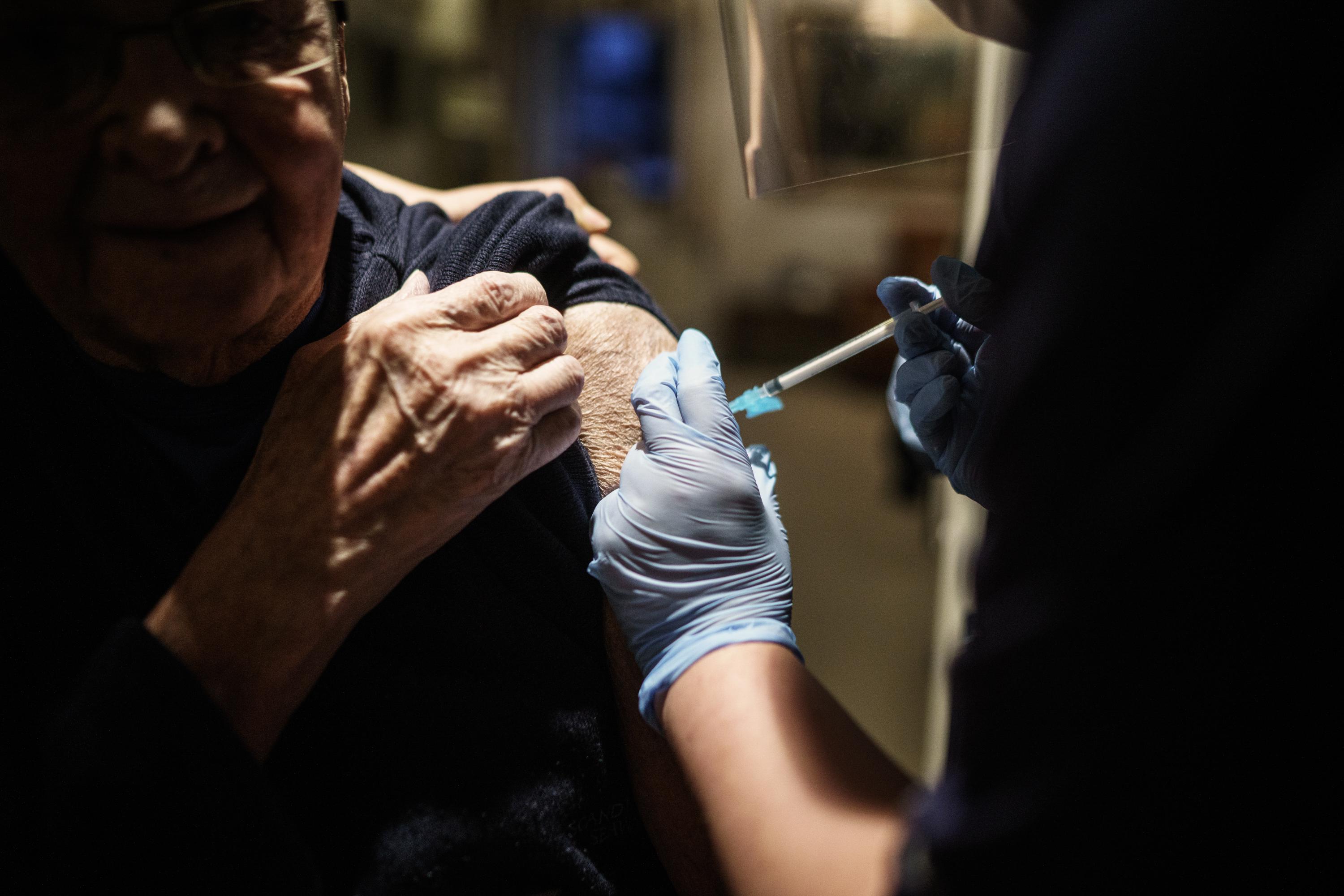
The vaccine will shorten the “shedding” time.
Beyond making up 70% of the world’s health workers, women researchers have been at the cutting edge of coronavirus research.
Could medical detection animals smell coronavirus?
Spoiler: Most people actually approved of their government’s approach.
Instead of looking forward, we should be consulting the past.
17th-century outbreaks of plague in Italy reveal both tensions between religious and public health authorities.
COVID-19 is a tragedy of the commons.
Not long after the COVID-19 pandemic caused colleges to start teaching remotely, students balked at the idea of paying full tuition for online learning. It’s not hard to understand why. […]
Despite unregulated face coverings being highly variable, they do, on average, reduce the spread of the virus.
President Vladimir Putin announces approval of Russia’s coronavirus vaccine but scientists warn it may be unsafe.
Pandemic-inspired housing innovation will collide with techno-acceleration.
Studying voice recordings of infected but asymptomatic people reveals potential indicators of Covid-19.
Vaccines find more success in development than any other kind of drug, but have been relatively neglected in recent decades.
Researchers at University College London link waist circumference with dementia.
In Chile, the so-called “release certificate” would free holders from all types of quarantine or restriction.
We will travel again, but it will not be the same.
R is a way of measuring an infectious disease’s capacity to spread.
Apps that warn about close contact with COVID-19 cases can help relax social distancing rules.
Men take longer to clear COVID-19 from their systems; a male-only coronavirus repository may be why.
Researchers argue that most coronavirus infections around the world go undetected.
Research supports wearing surgical face masks to slow the spread of the deadly coronavirus.
The response to the pandemic illustrates five actions we can take to address the global climate change crisis.
From a personal point of view and from an economic point of view, this is nothing short of potentially disastrous for people’s livelihoods.
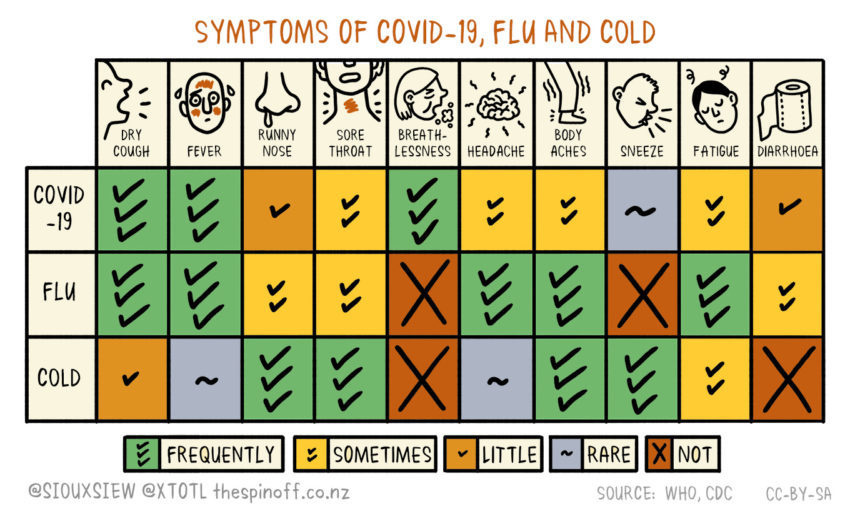
What symptoms to watch for, how to get tested, what to do if you’re sick, and when to go to the doctor.
Inequality from the Recession has a lot to do with how the government designed its response.
Half a billion people were infected.
A mission is planned for just three weeks from now, but NASA has a plan.