chemotherapy
A new study delivers the dark financial reality of cancer.
It neutralized not only the tumor it was injected into but malignancies all over the body.
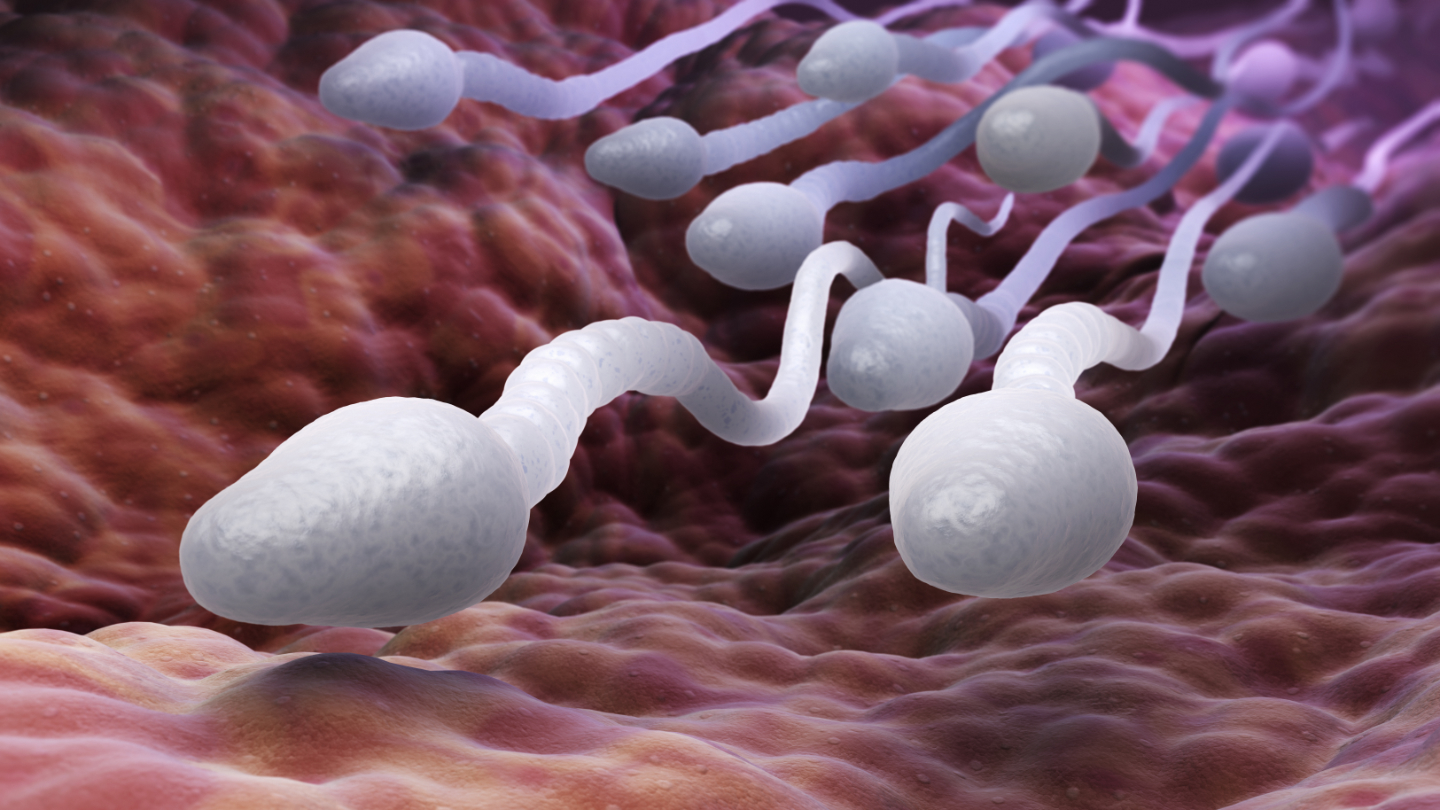
Researchers are studying the use of sperm cells as micromotors for delivering chemotherapy to cervical cancer patients.
This could end the days of suffering through cancer treatment.