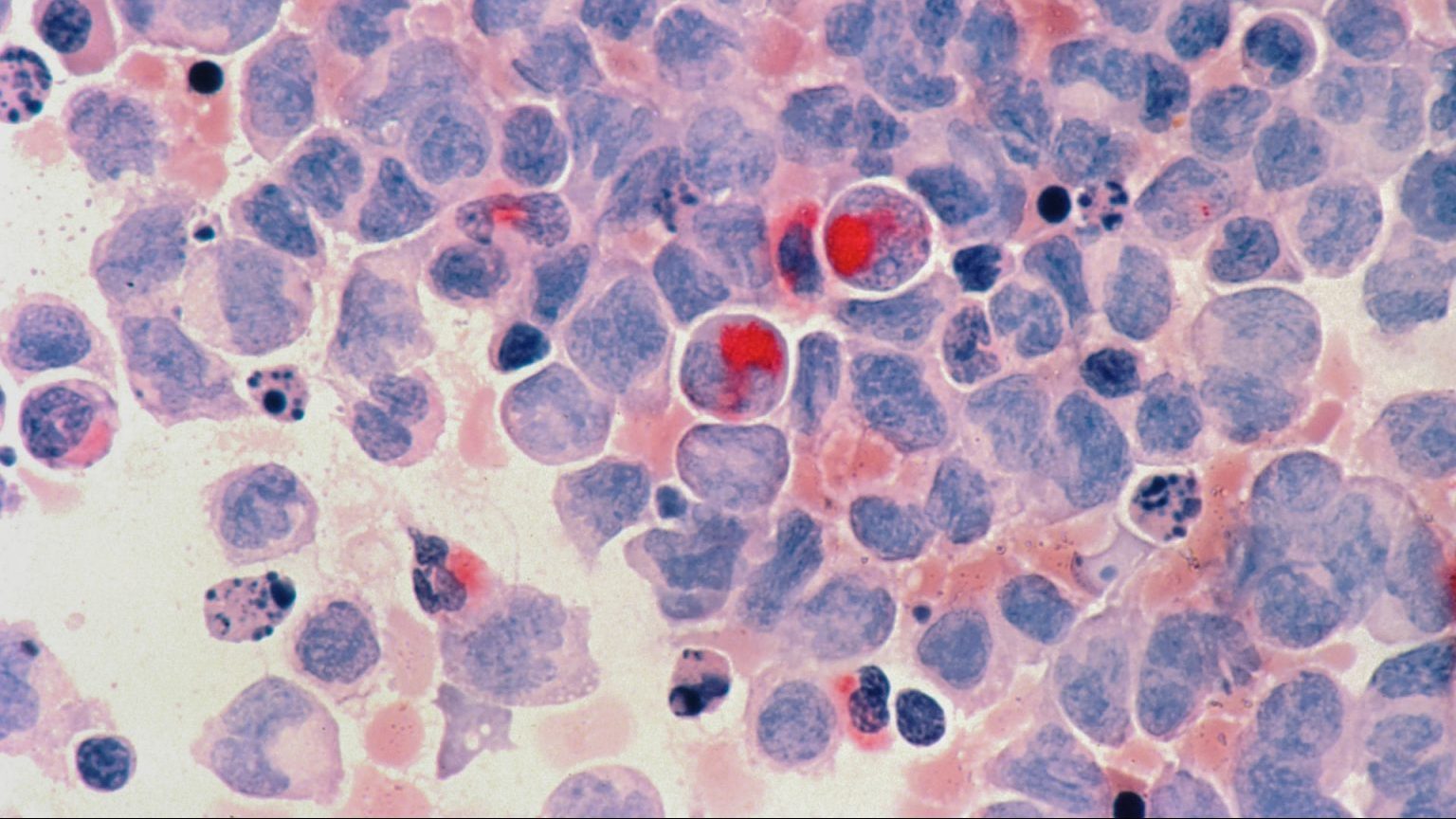
Evidence has been accumulating for some time that individuals with colorectal cancer (CRC) have an altered gut microbiome compared to healthy controls. Even so, it’s difficult to know whether the dysbiosis that occurs in individuals with CRC is a cause, or merely the result, of disease processes.
Work published earlier this month by researchers at the University of Michigan (Ann Arbor) and Baylor College of Medicine (Houston) may have settled that question. The researchers exposed germ-free mice either to feces and bedding materials from mice with CRC, or feces and bedding from disease-free mice, then subjected both groups to a tumor-inducing regimen involving intraperitoneal injection of azoxymethane (a potent carcinogen). Mice exposed to feces from cancerous peers were twice as likely to develop tumors as mice who got their germs from healthy peers, and in the latter case the tumors that did develop were fewer and smaller in size.
DNA analysis of recipient-mouse stool samples confirmed unambiguously that they had indeed acquired the respective microbiomes of the donor mice.
In one experiment, recipient mice were treated with antibiotics before and after exposure to bacteria from unhealthy (CRC) mice. Antiobiotic-treated mice had significantly fewer (and smaller) tumors than mice not so treated, tending to implicate the bacteria in tumorigenesis.
Said the authors of the study:
Our results demonstrate that changes in the gut microbiome associated with inflammation and tumorigenesis directly contribute to tumorigenesis and suggest that interventions affecting the composition of the microbiome may be a strategy to prevent the development of colon cancer.
Based on this and previous work implicating a Fusobacterium protein (FadA adhesin) in colorectal cancer, it’s beginning to seem pretty clear that CRC is, at least in part, a bacterial disease. If so, there’s probably a role for fecal transplants, antibiotics, and/or probiotics in the prevention and management of the ailment. Which is good news for everyone—except maybe Big Pharma (but I tend to think they’ll survive, regardless).
If you found this post useful, wont you please share it? Please tell friends and loved ones via Twitter, Facebook, etc. Thank you!