disease outbreaks
Prevention is always better than waiting .
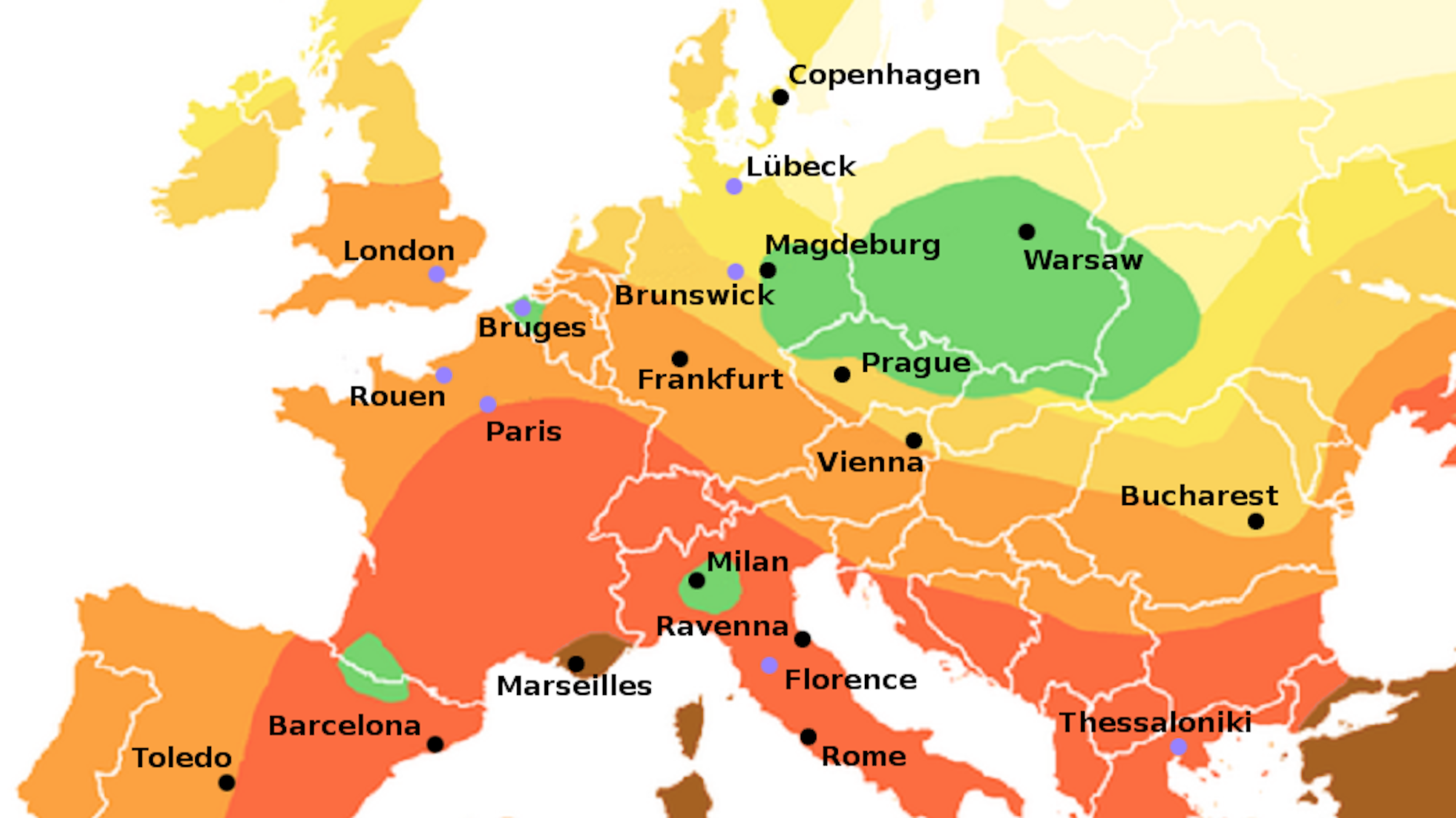
The Black Death skipped certain parts of Europe – and that could be a lesson for today’s coronavirus epidemic
Information is the best armor against panic.
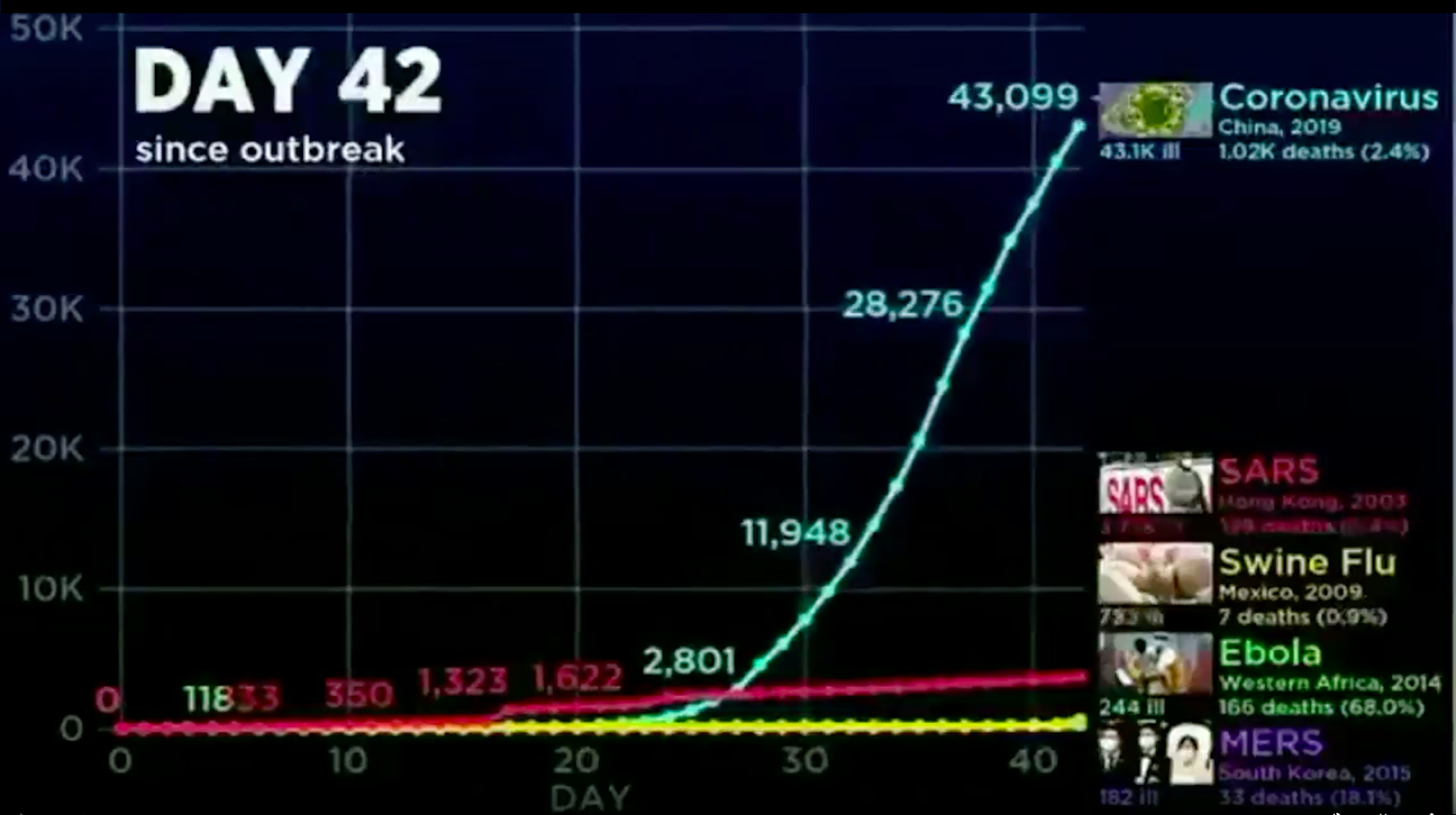
The video fragment only shows increase in COVID-19 cases, reversing the video’s original message to induce panic.
As the new coronavirus epidemic spreads, more and more people are wearing surgical masks—despite their questionable effectiveness. An anthropologist explores the reasons why.