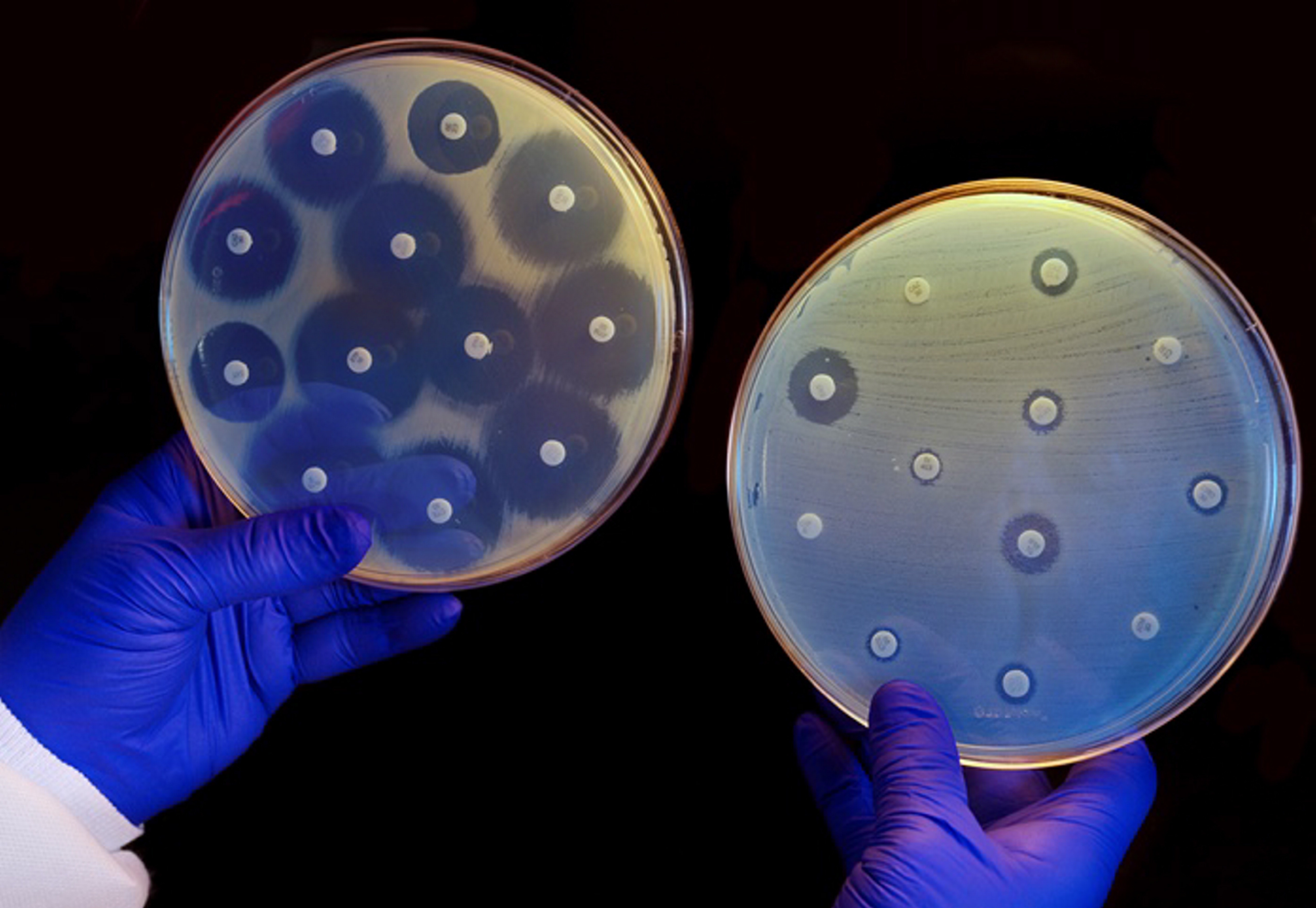
Microbes that live in our noses are able to kill MRSA, a superbug that has been resistant to various antibiotics. Researchers hope to use this discovery to develop new antibiotics.
Utilizing bacteria from within the human body to fight off antibiotic resistance is a new approach as most previous antibiotics have come from soil samples.
Initially, German researchers from the University of Tübingen found that the Staphylococcus aureus bacteria (some strains of which become the MRSA) is in about 30 per cent of the population, while the other 70 per cent did not have it. Further studies revealed that the reason for this lies in the Staphylococcus lugdunensis bacteria, which is able to fight off the other staph by creating its own antibiotic. This is the bacteria scientists are looking to harness to produce the new antibiotic they dubbed lugdunin.
So far the new antibiotic has been tested only on mice, defeating a number of bacteria which could cause diseases like meningitis, inflammation of the heart, as well as urinary tract and skin infections. Human trials are yet to be conducted.
“It’s really the first human-associated bacterium where the whole species is able to produce such an antibiotic,” said Bernhard Krismer, one of the study’s co-authors.
Professor Andreas Peschel, another co-author of the paper, explained how the scientists hope to make lugdunin into an effective drug:
“By introducing the lugdunin genes into a completely innocuous bacterial species we hope to develop a new preventive concept of antibiotics that can eradicate pathogens.”
While the discovery is exciting, developing a mass-produced version of the antibiotic can take a long time. In the meantime, antibiotic resistance is a growing problem that has the potential to lead to worldwide epidemics.
The overuse of antibiotics (particularly in the livestock we consume) has created the situation where resistant bacteria are threatening to become superbugs and cause fatal outbreaks of diseases we consider to be under control, like gonorrhea, tuberculosis and E.coli. A major reason for the issue is the lack of research and development by pharmaceutical companies which focus more on chronic conditions, finding it more lucrative to create drugs that a patient would be taking for years.
According to the CDC, more than 2 million Americans get infected every year due to drug-resistant antibiotics, with nearly 23,000 people dying. The number of people dying across the world is more than 700,000, including 214,000 infants less than a month old. A UK government report estimated that a superbug could kill 300 million people by 2050. Suffice it to say, the potential for a disastrous epidemic is definitely there.
You can read the paper here, in the journal Nature.