Two new studies identify whether cancer patients will respond to chemotherapy
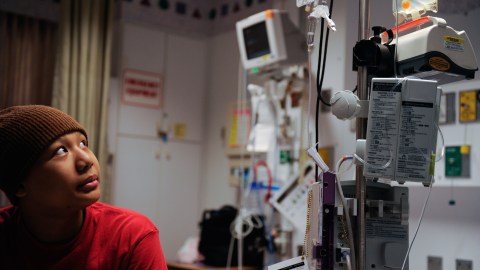
Mitchell Xayapraseuth receives chemotherapy at Providence Alaska Medical Center in Anchorage, Alaska in April 2012. (Marc Lester/Anchorage Daily News/MCT via Getty Images)
- Using radiomics, two new studies identified whether patients would respond to chemotherapy or not.
- This breakthrough occurred by investigating tissue around the tumor, instead of only looking at the tumor itself.
- This could lead to the cessation of much suffering for patients that will not respond to chemo.
We can thank warfare for one of the most important medical discoveries of the 20th century. An article published in TheNY Times in 1946 sums up a fascinating study on the usage of “nitrogen mustards”—mustard gas used by the Germans in Italy, which exposed over 1,000 people to the effects of the bombs—that led to trials conducted in New Haven on the potential of utilizing this chemistry in the treatment of Hodgkin’s disease (among other cancers).
The word ‘chemotherapy’ was coined by German-Jewish physician Paul Ehrlich over a century ago. It initially referred to the usage of chemicals to treat any disease, including antibiotics. Ehrlich was a bit of a medical savant, helping create treatments for syphilis and trypanosomiasis. He called his discoveries “magic bullets,” denoting the mortal specificity these drugs had on their biological targets. Beginning in 1904, he used a variety of arsenics, bromides, and alcohols to try to kill cancer cells.
In 1915, Ehrlich fell ill with tuberculosis. He was frustrated that his nation was using the chemicals he studied for healing in order to create weapons of war. Right before he died he looked out over plants operated by Bayer and Hoechst, which were creating what would become known as mustard gas, frustrated that his nation, on the eve of World War I, had gone so far astray.
While Ehrlich remained skeptical that a cocktail of lab-produced drugs could effectively combat cancer—his research resulted in weak or ineffective drugs—time proved to be his only problem. Trials conducted in America in 1942 showed efficacy in the treatment of lymphomas. From this research came mustine (chlormethine), first sold under the name Mustargen, to be employed in the treatment of prostate cancer.
Downsizing the fight with cancer | Efstathios Karathanasis | TEDxCWRU
Chemotherapy is a mixed bag—every cancer patient knows this. As with mustard gas bombs dropped over villages in hopes of rooting out enemies amid a civil population (and inevitable civilian casualties), chemo is often more of a guess than a specific application (though more targeted chemotherapies have been developed over the decades). Chemo doesn’t only destroy cancerous cells, it also halts the division of normal cells, resulting in immunosuppression, inflammation of the digestive tract, and hair loss.
While not a perfect medicine, few—though perhaps too many, at least in the conspiratorial holistic corners of the internet—doubt chemo’s efficacy, though they remain concerned about the side effects. When I went through testicular cancer five years ago, I was given three post-surgery options: one to two rounds of chemotherapy; radiation therapy (which can lead to a secondary cancer); or monitoring. I chose one round as prevention. There was nothing pleasant about it. Those who endure a dozen rounds for more aggressive cancers face a myriad of consequences from the suppression of their immune systems.
Yet the alternative is even less appealing. You can’t beat cancer as it’s an embedded part of us. Humans don’t exist without cancer cells. As physician and oncologist Siddhartha Mukherjee writes in his biography of cancer, The Emperor of All Maladies, cancer cells are “more perfect versions of ourselves.” To root them out entirely means to also destroy the cells necessary for making us human.
Every one of us lives with cancer cells. Whether or not the disease forms is dependent upon a host of factors, including genetics, diet, fitness level, exogenous factors (such as living near chemical plants or underneath flight pathways).
Regardless, having cancerous cells is a fate none of us escape. Mukherjee continues:
“The secret to battling cancer…is to find means to prevent these mutations from occurring in susceptible cells, or to find means to eliminate the mutated cells without compromising normal growth.”
Dr. Siddhartha Mukherjee: Genetically Mapping the Future of Cancer
There’s an art to the science of choosing the chemotherapy drugs included in a regimen; oncologists do not always choose correctly. This professional hurdle is slowly being overturned, thanks to research such as recent studies at Cape Western Reserve University that appear to have identified clues to whether or not a patient will respond to chemotherapy.
By scanning regions outside of the tumor observed on MRI and CAT scans, biomedical engineering professor Anant Madabhushi says that certain insights reveal whether lung and breast cancer patients will be benefited by chemotherapy.
One study sought a “signature,” known as HER2-positive, that is included in 20 percent of all breast cancers. Through radiomics, which uncovers quantitative features invisible to the naked eye, researchers can discover HER2 by analyzing tissue around the tumor. Instead of undergoing a “one-size-fits-all” course of chemotherapy, patients with this signature could be better targeted—though the researchers state a definitive breakthrough is a few years away.
In a corresponding study using radiomics, lung cancer researchers are on the verge of an important discovery. As biomedical engineering doctoral researcher, Mohammadhadi Khorrami, states, only one in four lung cancer patients respond to chemotherapy, meaning that 75 percent will endure unnecessary consequences and considerable pain because research thus far has been limited to investigating the tumor itself.
Through these investigative techniques, Khorrami identified, with 77 percent accuracy, which patients would benefit from chemotherapy, a nine percent increase over just looking inside the tumor. Considering 228,000 Americans will be diagnosed with the disease this year, that’s over 20,000 patients receiving better health care. As this particular regimen comes with a $30,000 price tag, a lot of financial and emotional strain can be saved through this new technique.
That we haven’t figured out a specific cure to the range of cancers we face is not surprising, but the fact that we’re gaining ground brings hope in the face of our species’ greatest killers. Cancer might be an inherent part of us, yet if we can mitigate the pain and suffering it wreaks, such research will be worth it.
—