Researchers stop COVID-19 drug trial after 11 patients die
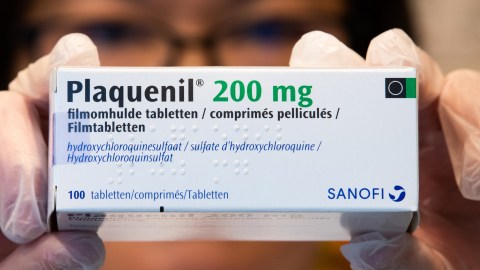
BENOIT DOPPAGNE / Contributor
- Scientists around the world are currently experimenting with chloroquine and hydroxychloroquine as potential treatments for COVID-19.
- Despite some early reports suggesting that these antimalarial drugs may help prevent and treat the disease, there’s still no solid evidence showing that they’re a safe and effective treatment.
- The recent trial in Brazil suggests that high doses of chloroquine are toxic and should be avoided.
A small clinical trial in Brazil suggests that one potential treatment for COVID-19 comes with life-threatening side effects.
As the world searches for effective COVID-19 treatments, some nations have authorized doctors to give patients antimalarial drugs as part of experimental clinical trials. These trials show some indication that the drugs, chloroquine and the closely related hydroxychloroquine, may be effective at treating and preventing COVID-19.
Early reports from China and France, for example, suggested that the drugs may help improve patients’ conditions. But health experts have cautioned against overhyping the results, flagging methodological issues in the research like not including a control group or having a small sample size. To date, there’s no solid evidence showing that these drugs effectively treat COVID-19 or block coronaviruses from infecting cells.
What is clear, based on previous research and the new trial in Brazil, is that these drugs can cause serious side effects, particularly among those with heart conditions.
“The antimalarial medication hydroxychloroquine and the antibiotic azithromycin are currently gaining attention as potential treatments for COVID-19, and each have potential serious implications for people with existing cardiovascular disease,” the American Health Association notes in a statement.
“Complications include severe electrical irregularities in the heart such as arrythmia (irregular heartbeat), polymorphic ventricular tachycardia (including Torsade de Pointes) and long QT syndrome, and increased risk of sudden death.”
In the recent Brazil trial, researchers gave chloroquine to 81 COVID-19 patients in a hospital in Manaus. The study involved two groups: One received a high dose of 12 grams of chloroquine over 10 days, the second group received 2.7 grams over five days. Both groups also received the antibiotic azithromycin, which poses its own heart risks.
By the sixth day of the trial, 11 patients had died, and the researchers decided to stop giving the drug to the high-dose group.
“Preliminary findings suggest that the higher chloroquine dosage (10-day regimen) should not be recommended for COVID-19 treatment because of its potential safety hazards. Such results forced us to prematurely halt patient recruitment to this arm,” the team wrote in a preprint paper.

Pedro Vilela / Stringer
The high-dose group had an especially high risk of suffering heart arrhythmias, a finding also observed in a separate trial on hydroxychloroquine conducted in a hospital in France, which cut the trial short.
“To me, this study conveys one useful piece of information, which is that chloroquine causes a dose-dependent increase in an abnormality in the ECG that could predispose people to sudden cardiac death,” Dr. David Juurlink, an internist and the head of the division of clinical pharmacology at the University of Toronto, told The New York Times.
Still, it’s possible that some combination of chloroquine, hydroxychloroquine and azithromycin may be effective at preventing and treating COVID-19. The researchers behind the Brazil trial said more research is “urgently needed,” but warned doctors against using high dosages.
“We therefore strongly recommend that this dosage is no longer used anywhere for the treatment of severe COVID-19, especially because in the real world older patients using cardiotoxic drugs should be the rule.”
One major problem in searching for COVID-19 treatments is that it’s currently difficult to conduct clinical trials in a normal and methodologically sound manner. Despite increasing demand for drugs like chloroquine, many health experts are warning that more research is needed to understand their effects and risks.
“The urgency of COVID-19 must not diminish the scientific rigor with which we approach COVID-19 treatment,” Robert A. Harrington, M.D., FAHA, president of the American Heart Association said in a recent statement. “While these medications may work against COVID-19 individually or in combination, we recommend caution with these medications for patients with existing cardiovascular disease.”